Expert Lung Cancer Treatment
by Dr. Marco Scarci
Dr. Marco Scarci combines over 20 years of thoracic expertise with a genuinely patient-centred approach. He takes time to explain your options, answer your questions, and make sure every decision feels right for you.
Every treatment plan is individually designed, reviewed by a full multidisciplinary team, and guided by the latest clinical evidence.

100+
Five-Star Reviews From Lung Cancer Patients
85-90%
Cure Rate for Stage I Lung Cancer With Early Surgery
1 Week
From First Consultation to Treatment
20+ Years
Specialising in Thoracic and Lung Cancer Surgery
5,000+
Minimally Invasive Procedures Performed
Lung cancer surgery involves the precise removal of cancerous tissue from the lung, with the aim of eliminating the disease while protecting as much healthy lung function as possible. It is the most effective curative treatment for early-stage lung cancer, and in many cases, it offers patients the best long-term outcomes of any available option.
Mr. Marco Scarci performs the full range of lung cancer surgical procedures in London, from small lung-sparing resections to complex operations involving multiple structures. The vast majority are performed using minimally invasive techniques, through a single 3cm incision, meaning less disruption to the body and a faster return to everyday life.
Lung cancer develops when abnormal cells in the lung grow and divide uncontrollably. It is one of the most commonly diagnosed cancers worldwide, but outcomes have improved significantly with advances in early detection and surgical techniques. The earlier it is caught, the more treatment options are available.
Non-Small Cell Lung Cancer (NSCLC)
The most common type, accounting for around 85% of all lung cancer cases. Cells tend to be larger and grow more slowly. Subtypes include adenocarcinoma, squamous cell carcinoma, and large cell carcinoma.
Small Cell Lung Cancer (SCLC)
A faster-growing form of lung cancer, accounting for roughly 15% of all cases. It often responds well to chemotherapy and radiation therapy. Identifying your type is key to building the most effective treatment plan.
Early-stage lung cancer often presents with no symptoms at all. If you have any concerns, or have one or more risk factors, seek advice promptly and discuss screening options with a specialist: early diagnosis makes a significant difference to outcomes.
The role surgery plays in your treatment depends on the stage of your cancer. Each stage presents different challenges and different opportunities, and understanding where you are in that picture is the first step towards finding the right path forward.
Here is what that means in practice.
Early Victory
The cancer is contained within the lung. Surgery alone can be curative, with survival rates exceeding 85 to 90%. Most patients are home within one to two days.
Still Strong
The cancer may have spread to nearby lymph nodes. Surgery remains central, and is combined with chemotherapy, radiotherapy, or immunotherapy. Full remission is achievable.
More Complex
At this stage, cancer may spread to the lymph nodes or chest wall. Surgery becomes one part of a coordinated treatment plan, reviewed and approved by a full specialist team.
Comfort Comes First
When cancer has spread beyond the chest, palliative surgery can still make a real difference. It can help relieve symptoms, support your comfort, and improve your overall quality of life.
Not sure which stage applies to you?
You do not need to piece it together alone. Dr Marco Scarci will review your case in full, explain your options clearly, and help you understand exactly what treatment can offer you.
Every patient is different, and so is every operation. Dr. Scarci will take the time to understand your individual situation, your health, and your priorities before recommending the most appropriate procedure.
His approach is always guided by the latest clinical evidence, reviewed by a full multidisciplinary team, and tailored to your specific tumour, lung function, and overall wellbeing.
The goal is always to remove the cancer as thoroughly as possible whilst preserving as much healthy lung tissue as he can, giving you the best chance of a full and active recovery.
The type of surgery recommended will depend on the size and location of your tumour, how much of the lung is affected, and how well your lungs are currently functioning. Dr Scarci will review your scans and overall health before recommending the procedure that is right for you. Here is an overview of the three main surgical options available:
Lobectomy
One complete lobe of the lung is removed. The remaining lobes continue to function normally after surgery.
The gold standard treatment for non-small cell lung cancer. The most frequently performed lung cancer operation worldwide.
With minimally invasive techniques, most patients are home in one to two days and back to normal activities within weeks.
Pneumonectomy
The entire lung, either left or right, is removed. The remaining healthy lung takes over full respiratory function over time.
Advanced cases where the cancer spans multiple lobes and cannot be addressed with a smaller, more targeted resection.
Reserved for cases where no other surgical option is appropriate. One healthy lung is sufficient to support a full and active life.
Lung-Sparing Surgery
Smaller, targeted procedures that remove only the affected area of the lung, leaving as much healthy tissue intact as possible.
Small, early-stage tumours where protecting lung function is the priority and a full lobe removal is not necessary.
The least invasive surgical option available. Patients typically recover quickly and retain strong breathing capacity after the procedure.
The majority of Dr Marco Scarci’s operations are performed using minimally invasive techniques. This means smaller incisions, less pain, faster recovery, and a shorter hospital stay compared to traditional open surgery.
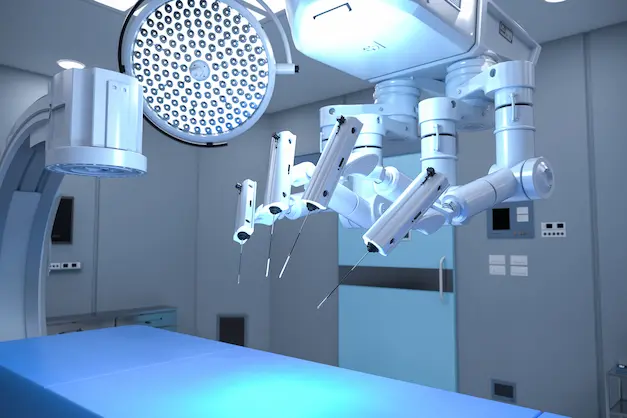
How it Works:
The surgeon controls robotic arms with exceptional precision from a console, enabling highly controlled, fluid movements in areas of the chest that are difficult to reach.
Best for:
Complex or anatomically challenging cases where a higher degree of precision and visualisation is required.
Benefits:
Superior accuracy, reduced risk of complications, and excellent outcomes in cases that would be difficult to perform with standard minimally invasive techniques.
How it Works:
The surgeon controls robotic arms with exceptional precision from a console, enabling highly controlled, fluid movements in areas of the chest that are difficult to reach.
Best for:
Suitable for the majority of lung cancer operations, including lobectomy, segmentectomy, and wedge resection.
Benefits:
Less disruption to the body, significantly reduced post-operative pain, and a faster return to everyday life compared to traditional open surgery.
How it Works:
The entire operation is performed through a single 3cm incision. All instruments and the camera enter through the same small opening, making this the most advanced form of minimally invasive lung surgery currently available.
Best for:
Patients who are suitable candidates for minimally invasive surgery and want the fastest possible recovery with the least disruption to their body.
Benefits:
25% of patients go home on day one. 50% go home on day two. Minimal scarring, reduced pain, and the fastest recovery of any surgical approach available.
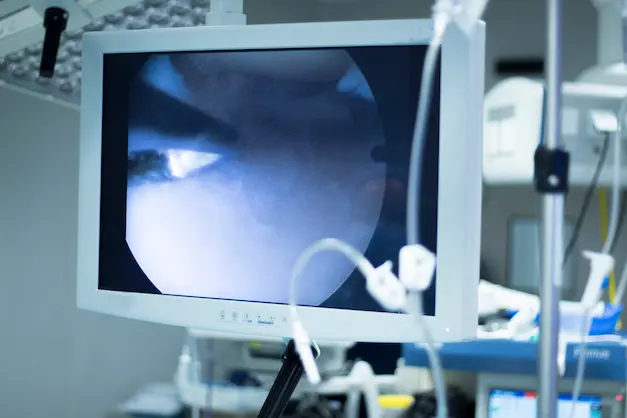
How it Works:
A small camera is passed through a keyhole incision, giving the surgeon a clear, detailed view inside the chest without the need to open it fully.
Best for:
Early to mid-stage lung cancer where a minimally invasive approach is appropriate and the tumour is accessible.
Benefits:
Shorter hospital stays, typically two days compared to one week for open surgery, with minimal scarring and less post-operative discomfort.
Understanding your surgical options is the first step towards feeling in control. When you meet Dr Marco Scarci, he will bring all of this together in the context of your specific diagnosis and help you move forward with clarity and confidence.
We know that uncertainty can be one of the hardest parts of facing lung cancer surgery. Knowing what lies ahead makes everything feel more manageable. Here is exactly what you can expect at every stage of your journey with Dr Scarci, from your very first appointment through to your recovery and beyond.
Initial Consultation
Your journey begins with a thorough one-to-one consultation with Dr Marco Scarci. He will listen to your symptoms, review your medical history, and go through any existing test results. This is your opportunity to ask questions and understand what comes next.
Diagnostics and Imaging
A full picture of your condition is built before any decisions are made. This typically includes a CT scan, PET scan, lung biopsy, genetic and biomarker testing, and lung function tests to assess the tumour and how well your lungs are working ahead of surgery.
Team Review
Your case is reviewed in full by a dedicated multidisciplinary team including Dr Scarci, a medical oncologist, and a specialist radiologist. Every scan and aspect of your diagnosis is reviewed carefully together by the full team before a recommendation is made.
Your Treatment Plan
Dr Marco Scarci will walk you through the recommended plan in full, including the type of surgery, the timing, and whether any pre-operative treatment is needed. Every option is explained clearly and honestly, and every decision is made with you, not for you.
The Operation
Most procedures are performed using minimally invasive techniques through a single small incision. The operation typically takes two to three hours under general anaesthesia, with a focus on removing the cancer whilst protecting as much healthy lung tissue as possible.
Hospital Recovery
Most patients are encouraged to walk on the same day as their operation. Once your chest drain has been removed and your team is satisfied with your progress, you will be ready to go home. For most patients, discharge happens within one to two days of surgery.
Recovery and Monitoring
Your journey begins with a thorough one-to-one consultation with Dr Marco Scarci. He will listen to your symptoms, review your medical history, and go through any existing test results. This is your opportunity to ask questions and understand what comes next.
Recovery from lung cancer surgery is different for every patient, but knowing what to expect at each stage makes the process far less daunting.
Dr Scarci and his team will support you closely from the moment you wake up after surgery to your return to normal life.
Most patients walk on the same day as their operation. Pain is managed using nerve blocks and cryoanalgesia, and breathing exercises begin early. Most patients are home within one to four days.
Energy returns steadily and light daily tasks become manageable. Most patients return to light work from week two. A follow-up appointment with Dr Scarci takes place during this period.
Most patients are back to driving, socialising, and gentle exercise by month two. Surveillance scans monitor progress and lung function continues to improve steadily through to month six.
Why Choose Dr Marco Scarci?
Choosing the right surgeon is one of the most important decisions you will make. Mr Marco Scarci combines world-class surgical expertise with a genuinely personal approach, ensuring you feel informed, supported, and confident at every stage of your care.
Focused on Curing Every Patient
Every operation is approached with one goal in mind: to remove all cancer cells and give each patient the best possible chance of a full recovery.
Early Surgery Can Save Your Life
Early lung cancer surgery can restore your normal life expectancy. The sooner your cancer is treated, the greater the opportunity to return to a full, active, and unrestricted life.
Evidence-Based Decisions
Surgery is only recommended when it offers a clear survival advantage, backed by solid clinical evidence, and approved by a full multidisciplinary team.
Minimally Invasive Surgery
Most operations are performed through a single 3cm incision or robotic-assisted surgery. The approach is always chosen based on what is best for you.
No Hidden Costs, No Surprise Bills
Fee-assured with all major insurers, as are the anaesthetists he works with. If you are paying directly, all follow-up appointments are included in the cost of your treatment.
He Takes On High-Risk Cases
Mr Scarci and his team regularly takes on cases other surgeons consider too high-risk, delivering successful outcomes where others have said no.
I spoke to Dr Narco yesterday regarding my health condition. He was very helpful and supportive.
03/31/2026 | Source: Top Doctors UK
Dr Scarci is very caring and takes the time to listen to your concerns and explain them. He is very prompt and knowledgeable in multi disciplinary endometriosis.
03/25/2026 | Source: Top Doctors UK
03/21/2026 | Source: Top Doctors UK
No. Early stages often benefit most. Advanced cancers may need other treatments, sometimes together with surgery.
Many early-stage patients are cured by surgery, but advanced-stage patients can also be cured by combining different treatment modalities.
Most take 2–3 hours.
A few weeks to a few months, depending on the type of surgery.
Modern techniques minimise bleeding, scarring, and pain.
It's best for early-stage patients. Eligibility depends on tumour size, location, and overall health.
It offers superior precision and recovery, especially in expert hands, but there is no clinical evidence that it is significantly better.
Not significantly. Modern pain management is very effective.
Most return to normal activities within weeks. Driving is often cleared at 4–6 weeks.
Regular checkups and post-surgery imaging help track recovery.
Yes. Especially in Stage II and III cancers.
I practice according to the latest guidelines from international bodies such as the National Institute for Clinical Excellence, National Comprehensive Cancer Network, ESTS, British Thoracic Society, among many others. My mortality is lower than the national average, and my length of stay is 25% shorter than the national average.
Call, email, or use the contact form. We prioritise fast access for urgent cases.