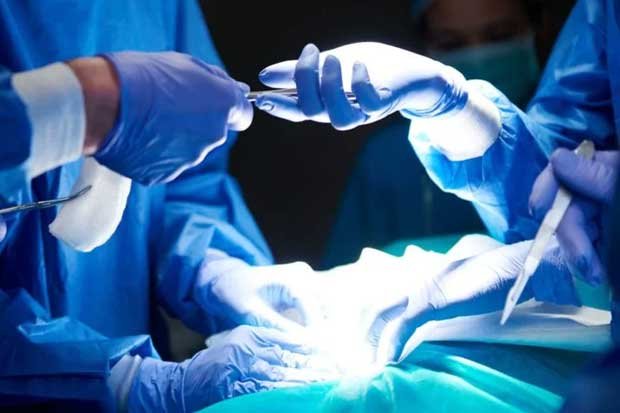
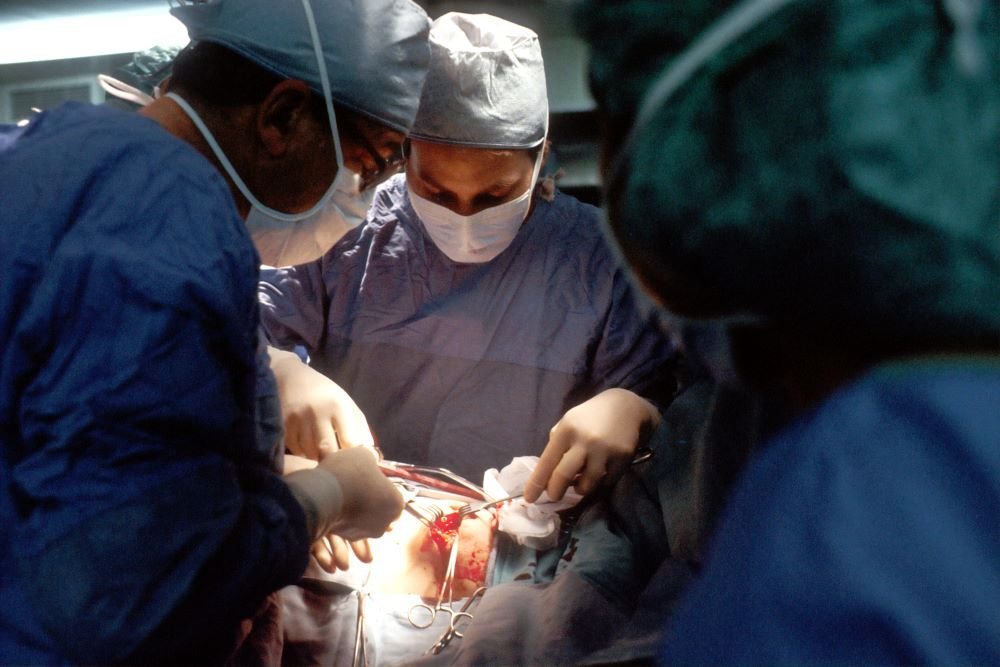
Recovering from cancer surgeries brings peculiar challenges that patients have to face. Surgical approaches for cancer require close monitoring of several factors. Collectively, these factors determine the overall health outcome for the patients. Keyhole lung cancer is performed routinely by Mr Scarci with just one single cut of 3cm. Such approach determines a faster recovery, reduced hospitalization and readmissions, and improved patient care in the postoperative period. In my practice about 25% of patients go home on the first post-operative day and about 50% on the second postoperative day. These results are due to the principle of “incremental gains”, in other words my team and I put together all the interventions and innovations, doesn’t matter of small, so that together generate significant benefits for the patients. Resection of a part of the lung can seem a daunting prospect, but nowadays, thanks to the most advanced keyhole techniques, the impact is not what it used to be and indeed there has been an overall increase in patients being offered surgery compared to few years ago, this is simply because we got so much better at dealing with pre-operative conditions and are surgery is a lot less aggressive than it used to be.
Will I be able to breath as well as before? Will I be short of breath? Will I need to carry around an oxygen cylinder?
Questions like those above come up almost in every consultation with my patients, although there isn’t a one size fits all answer for all patients, we can say that generally when we decide to operate we expect that the patient will be able to return to a good quality of life afterward.
Traditionally recovery after lung resection usually takes up to 3 months, although many patients are able to resume normal activities and be considered for additional treatment (either chemotherapy or immunotherapy) within few weeks.
Do you think I/my relative are too old for surgery? Do you think is worth having surgery at my age?
Again I am asked this a lot. Usually we offer surgery when there is a significant survival advantage. That means that if we manage to eradicate the cancer surgically the patient has a good chance of living his normal life expectancy. Surgery will inevitable impact, in the short term, on the quality of life, but usually this is transient. Modern anesthetic and surgical techniques made possible a recovery that was unimaginable only few years ago.
Is there any alternative to surgery? Do I have to have this operation even if I don’t like it/don’t feel ready?
Surgery is a form of treatment that we offer after thoughtful deliberation in what is a called an MDT, a short form for multidisciplinary team meeting. This is a meeting where many specialists that deal with lung cancer meet regularly and discuss each single case to come to a consensus opinion on what is the best treatment for each individual patient. If you are offered surgery you can be assured that this is going to be the best treatment for you. The best treatment though does not mean the only one. Patients’ a view is extremely important and shared decision making is at the heart of all we do, after all we are going to be partner in care during your treatment. If you don’t want surgery you might be offered other forms of treatment such as stereotactic radiotherapy or, in his fancy commercial name, cyber knife. The name here is misleading as there is no knife as such involved, only high dose radiations targeted onto the nodule in the lung. If you opt to discuss such treatment you will meet a specialist that will go through what it entails in detail.
Will I need any further treatment after my operation?
This is a very interesting question and usually it depends on the stage of the cancer. Usually earlier stages, so far, have not received any additional treatment, but increasingly patients in that category are being offered immunotherapy treatment to reduce the risk of the cancer coming back. More advanced stages will almost always need further treatment. This is something that will be discussed at the MDT with the result of the analysis of the specimen removed at surgery. You will then meet an oncologist to discuss options.
Do you crack my ribs? How long will it take for the scar to heal?
One of the advantages of keyhole surgery is that ribs are not spread apart. This reduces dramatically the amount of pain after surgery. Moreover, in my practice, I perform surgery with just one 3cm incision. This particular technique reduces the chance of nerve injury thus further decreasing the post-operative pain. One of the most satisfying things about my job is when patients ask me in the postoperative recovery room if they have been operated on as they don’t feel pain. Thankfully I get asked this question a lot.
What to eat after surgery? Is there a particular diet to avoid the cancer coming back?
There isn’t a particular diet suggested after surgery, the word here is moderation. You can eat pretty much anything you want giving preference to protein rich food (meat, eggs, fish), plenty of fruit and vegetables and trying to avoid un-healthy, prepacked food. Generally speaking anything that swam, ran or grew is good for you.
I feel stressed about my surgery, under the weather, can’t get my energy back.
Surgery has a big impact. Even if the scar is small the operation inside is the same as with a big scar. A good way to cope with the surgery is to acknowledge that it is ok to be scared. The next step is to realise that help is all around you. Speak to your surgeon and/or lung cancer specialist nurse. They will be able to provide support directly and relief your anxiety, occasionally you might be prescribed tablets or refer to clinical psychology for further support.
It is also normal not to be as energetic as before and struggle to do tasks that were very easy before surgery. The way to go here is to take it easy, listen to your body and let it recover whilst pushing slightly the boundaries every day. I always tell my patients that the bed and the armchair are their enemies. I expect them to go about for a daily walk, starting with 5 minutes a day and increasing by a minute every day, from the day after the discharge. This is a minimum and if a patient feels that can do more that is perfectly fine. A good rule of thumb here is to walk at the pace that feels like working out but still able to maintain a conversation. In other words the pace should be such that you are not out of breath nor find it too easy.
Lastly I would like to stress the importance of the people around you. Let them help you, all my patients have an in-depth conversation before surgery so that they know what to expect, how to cope with the immediately postoperative period and also I am always contactable by phone in case of any emergency.
If you have lung cancer contact Dr. Marco Scarci for your initial consultation and he will be able to help you.